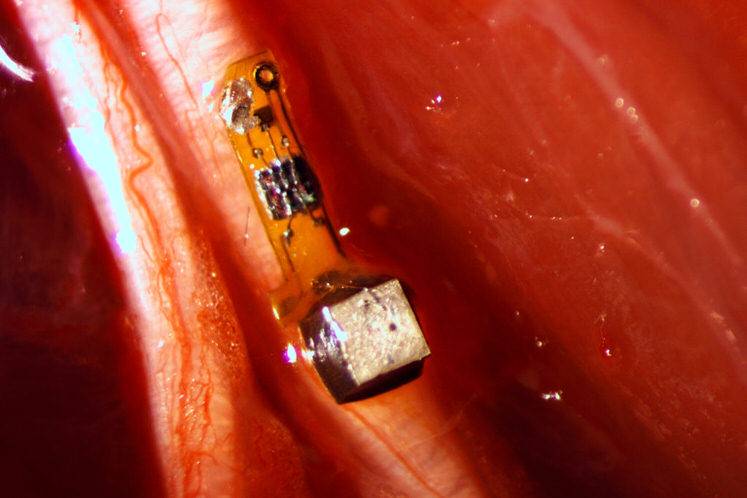
The notion of smart dust sounds like a work of science fiction but scientists at University of California Berkeley have developed a “neural dust” that can be implanted into the body, to monitor internal nerves, muscles or organs in real time.
The sensors are about the size of a large grain of sand contain a piezoelectric crystal that converts ultrasound vibrations from outside the body into electricity to power a tiny, on-board transistor that is in contact with a nerve or muscle fiber. A voltage spike in the fiber alters the circuit and the vibration of the crystal, which changes the echo detected by the ultrasound receiver, typically the same device that generates the vibrations. The slight change, called backscatter, allows them to determine the voltage.
See also: For new e-skin products, plastics are the future
The research could one day lead to brain machine interfaces for controlling prosthetics and robotics as well as faciliate a new biohealth industry of “electroceuticals.”
“The original goal of the neural dust project was to imagine the next generation of brain-machine interfaces, and to make it a viable clinical technology,” said neuroscience graduate student Ryan Neely. “If a paraplegic wants to control a computer or a robotic arm, you would just implant this electrode in the brain and it would last essentially a lifetime.”
Contemporary implantable electrodes degrade within 1 to 2 years, and all connect to wires that pass through holes in the skull. Wireless sensors could be sealed in stopping unwanted movement of the electrodes and prevention of infection.
Is smart dust the pinnacle of IoT creativity?
Research by Gartner into ‘hype cycles’ within emerging technology predicts that Smart Dust will become trend within 5 to 10 years. It’s a field that has been developing within research laboratories since the late 1990’s, with funding by the Defence Advanced Research Projects Agency (DARPA) to create applications of military relevance, their work involving “evolutionary and revolutionary advances in miniaturization, integration, and energy management.”
As early as 2003, researchers were working on applications for smart dust, which they characterised “tiny wireless microelectromechanical sensors (MEMS) that can detect everything from light to vibrations”. Commercial applications considered included serving as traffic sensors in congested urban areas and monitoring the power consumption of household appliances to determine whether they’re operating at peak efficiency. However, scientific advances have moved the smart dust motes from everyday sensor technology applications to implanted wearable devices.
According to neuroscientist Jose Carmena:
“The beauty is that now, the sensors are small enough to have a good application in the peripheral nervous system, for bladder control or appetite suppression, for example. The technology is not really there yet to get to the 50-micron target size, which we would need for the brain and central nervous system. Once it’s clinically proven, however, neural dust will just replace wire electrodes. This time, once you close up the brain, you’re done.“
The team at work to miniaturize the device further, find more biocompatible materials and improve the surface transceiver that sends and receives the ultrasounds, ideally using beam-steering technology to focus the sounds waves on individual motes. They are now building little backpacks for rats to hold the ultrasound transceiver that will record data from implanted motes.
“Dust” could also detect chemical levels
They’re also working to expand the motes’ ability to detect non-electrical signals, such as oxygen or hormone levels.
“The vision is to implant these neural dust motes anywhere in the body, and have a patch over the implanted site send ultrasonic waves to wake up and receive necessary information from the motes for the desired therapy you want,” said Dongjin Seo, a graduate student in electrical engineering and computer sciences. “Eventually you would use multiple implants and one patch that would ping each implant individually, or all simultaneously.”
The biggest barrier to the mainstreaming of smart dust is perhaps the reality that at present, it requires surgical implanting. Will it be possible in the future to swallow or inhale the dust? Our digestive system makes it highly questionable, but it’s an interesting idea. At any rate, as the dust gets smaller, it’s entry into the central nervous system and brain could lead to life changing interventions for people with particular health conditions and disabilities. It’ll be a way off, but if the research so far is anything to go by, it’s inevitable.